Under the Affordable Care Act, you have the right to have an external expert review your disputes with your health insurer. In 2019, Molina has repeatedly manipulated, blocked and stalled my requests for independent review, also called an IRO.
IMPORTANT: If you’ve had serious problems with Molina (of any kind), please fill out this short survey to help me gather information about the company’s harms. Together, we may be able to take further action.
Earlier I wrote about how a number of firms that are paid to perform independent reviews may be rigging the results in favor of insurers, well for consumers insured by Molina, there are even more levels of interference.
It appears from public health insurance data from Washington State, that Molina may be systematically blocking independent review requests by their members, potentially violating their federal rights.
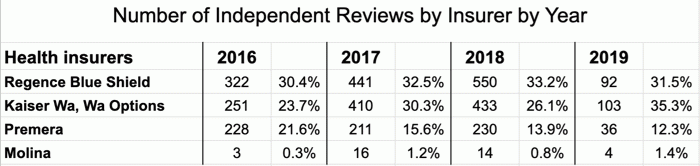
Using the Washington State’s Office of Insurance Commissioner’s Independent Review data reporting tool, I compiled independent review numbers for the top insurance companies in Washington.
While Regence, Kaiser and Premera Blue Cross pay for hundreds of independent reviews each year, Molina barely performs any. This aligns with my experience throughout 2019 in which Molina manipulated my first two requests and blocked all of my subsequent requests.
The insurance commissioner, Mike Kreidler, and his staff have been complicit and allowed Molina to do this without providing any explanation as to how Molina complies with federal ACA rights.
Even the commissioner’s own website and public guides (pdf) describes insured consumers’ rights to independent reviews.

I’ve been aghast all year at the horrible experience I’ve had with both Molina and the commissioner’s staff. It’s like they don’t read their own materials (and I have asked them):

It’s pretty darn clear at Healthcare.gov:

Text moved for image clarity. Original link.
Here’s the federal Department of Health and Human Services (DHHS)’ “Guidance On External Review For Group Health Plans And Health Insurance Issuers” (pdf):
These 16 minimum consumer protection standards…
1. The process must provide for external review of adverse benefit determinations (and final internal adverse benefit determinations) based on medical necessity, appropriateness, health care setting, level of care, or effectiveness of a covered benefit.
2. Issuers (or plans) must be required to provide effective written notice to claimants of their rights to external review.
3. If exhaustion of internal appeals is required prior to external review, exhaustion must be unnecessary if – (a) the issuer (or plan) waives the exhaustion requirement; (b) the issuer (or plan) is considered to have exhausted the internal appeals process by failing to comply with the requirements of the internal appeals process except those failures that are based on de minimis violations that do not cause, and are not likely to cause, prejudice or harm to the claimant5; or (c) the claimant simultaneously requests an expedited internal appeal and an expedited external review.
4. The cost of an independent review organization (IRO) to conduct an external review must be borne by the issuer (or plan), although the process may require a nominal filing fee6 from the claimant requesting external review. …
Department Of Health & Human Services’ Guide on External Review to Health Insurers (pdf)
Share Your Story with Me
I am collecting complaints from people insured by Molina Healthcare.
If Molina has blocked your requests for independent reviews (IRO), please fill out the survey. It’s very brief.
Also, if you received a surprising bill for out of network care at an in network provider or facility or you received an anesthesia bill for surgery at Swedish, please definitely, fill out the survey.
I will be writing more about the Washington State health insurance system and Molina soon. Keep up to date by following me on Twitter or subscribing to my blog using the form on the right, or at the bottom.

Share this: